In emergency and trauma care, time is critical. Decisions must be made quickly, often under pressure, and with limited information. One of the key questions in vascular trauma and reconstructive procedures is simple — yet crucial:
Is blood flow restored?
While imaging techniques and clinical experience guide treatment, the ability to objectively assess perfusion in real time can significantly improve decision-making.
The Challenge in Trauma and Vascular Surgery
In trauma cases involving vascular injury, compromised blood flow can lead to severe complications, including tissue damage, delayed healing or even limb loss.
After surgical intervention — such as revascularization — clinicians need to confirm that circulation has been successfully restored.
However, traditional methods often rely on:
-
visual inspection
-
palpation of pulses
-
indirect indicators
These approaches can be subjective and may not reflect microcirculatory perfusion, especially in distal regions such as the toes.
Real-Time Perfusion Assessment at the Point of Care
Modern optical measurement techniques allow clinicians to assess tissue perfusion directly at the site of interest. By using optical sensors placed on the toes, it becomes possible not only to detect the presence of blood flow, but also to assess perfusion pressure and monitor changes immediately after an intervention.
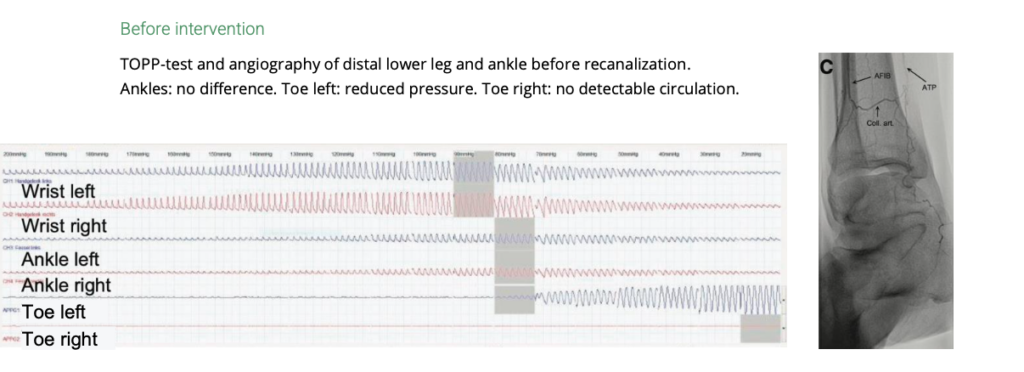
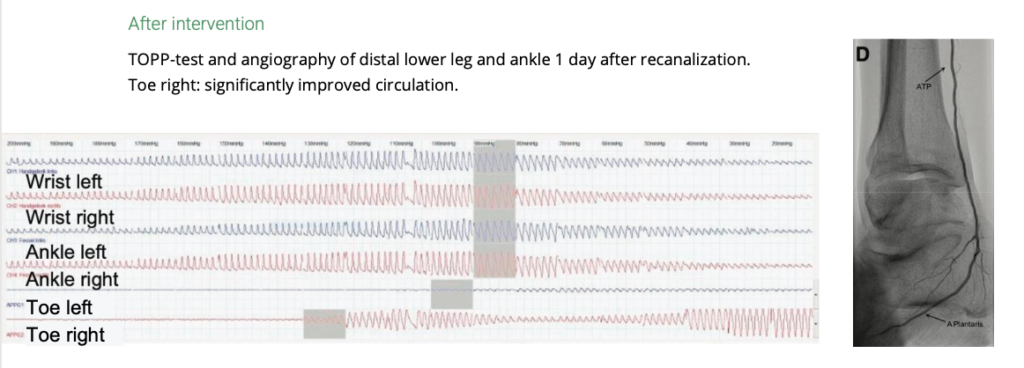
Clinical Insight: Before and After Revascularization
A clinical case demonstrates the value of real-time perfusion assessment in a patient with severely impaired pedal circulation due to arterial occlusion. Before intervention, measurements at the ankle level showed no significant side differences, which could suggest preserved macrocirculation. However, at the level of the toes, the situation was markedly different: reduced pressure was observed on the left side, while no detectable circulation was present in the affected right toe. Following revascularization, perfusion in the previously affected toe could be clearly measured, indicating a significant improvement in microcirculation and confirming successful restoration of blood flow.
This case highlights the importance of assessing not only large vessel flow but also distal microcirculation. Real-time measurement at the point of care provides immediate, objective feedback and supports both intraoperative and postoperative decision-making.
Expanding the Use Case: Beyond PAD and Diabetic Foot
While vascular diagnostics are commonly associated with PAD or diabetic foot, their role in trauma care is increasingly relevant.
In emergency and surgical settings, rapid and reliable perfusion assessment can:
-
support decision-making in the ER
-
guide intraoperative evaluation
-
reduce uncertainty after intervention
-
improve patient outcomes
Integrated Vascular Diagnostics
Comprehensive vascular assessment — including both arterial and microcirculatory evaluation — can be performed using integrated systems such as AngE™ ABI+.
By combining oscillometric measurements with optical perfusion assessment at the toe, clinicians gain a more complete picture of vascular status in a single workflow.
👉 Learn more and download our guide: https://www.sot-medical.com/how-to-reliably-detect-pad-in-3-minutes-guide/
Conclusion
In time-critical situations, objective information matters.
Real-time perfusion assessment provides clinicians with immediate insight into vascular status — helping to confirm treatment success and support better clinical decisions.
When every second counts, reliable diagnostics can make a meaningful difference.

